Total Hip Replacement – Fast Facts
Are you considering having total hip replacement surgery? These fast facts from Dr Dan Fick will help you find out more about the procedure before you chat to your orthopaedic surgeon.
What Is a Total Hip Replacement?

A total hip replacement is a type of orthopaedic surgery designed to replace a worn out and damaged hip joint with an artificial joint known as a prosthesis or prosthetic joint.
You might hear a surgeon talking about total hip arthroplasty – this is just another name for hip replacement.
Total hip replacement surgery is recommended for people with disabling hip pain that has not improved with other treatments such as anti-inflammatory pain medication, physiotherapy or lifestyle changes such as increased activity or weight loss.
Why Should I Consider Total Hip Replacement?
A hip replacement can reduce the joint pain you may have been experiencing, improve your mobility so you can walk and move around with ease, and improve your quality of life so you can get back to doing the things you enjoy.
What Happens During Total Hip Replacement Surgery?
In general, total hip replacement surgery takes about 1 hour. To have the surgery, you will need to have a local anaesthetic and a spinal anaesthetic which will numb your lower body during the procedure.
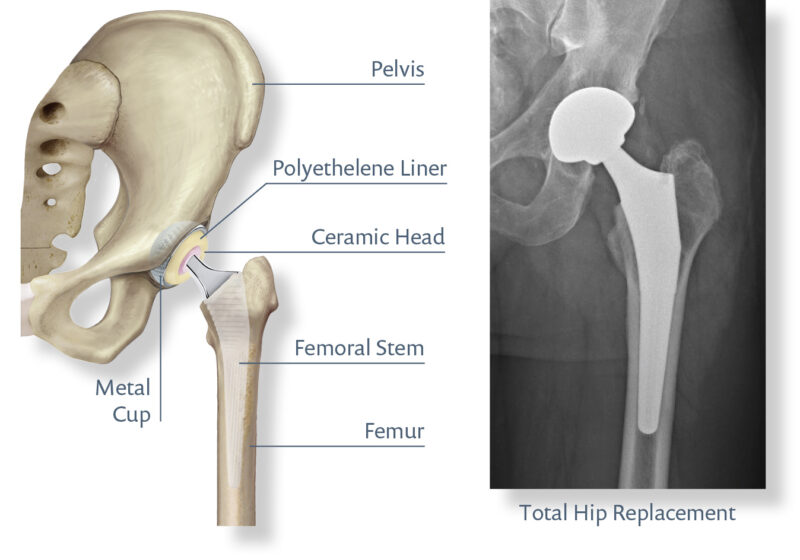
Total hip replacement surgery involves replacing the head of the femur (the ball at the top of the thigh bone) and the acetabulum (the hip socket) that is worn or diseased with artificial material.
The artificial stem is made of metal, the ball is made of ceramic, and the artificial socket is made of a durable, wear-resistant plastic liner (polyethylene) inside a metal-backed cup.
The ball and insert are designed to glide together to copy the body’s natural hip joint movement.
The surgical incision will be towards the back of your hip, usually about 10–15 cm long and your skin is usually closed with dissolvable sutures and a waterproof dressing.
What Are the Risks and Complications of Total Hip Replacement Surgery?
All surgery has some risks and your decision to have surgery should involve an informed discussion with your surgeon about how the benefits outweigh the potential downsides.
Here are some risks and potential complications of total hip replacement surgery that you should be aware of.
Infection:
This is a risk with any surgical procedure. In some cases, an infection may require further surgery to clean out the joint or remove the implant.
Blood clots (deep vein thrombosis or DVT):
DVT can be a serious and potentially life-threatening complication. Your medical team helps minimise the risk by recommending medications and/or compression stockings.
Leg length discrepancy:
The new implant may shorten or lengthen the limb so one leg may feel shorter than the other. We minimise the risk of limb length changes by making joint stability a top priority.
Dislocation:
With standard hip joints, there is a risk that the hip joint may become dislocated, especially during the early stages of recovery. However, Dan uses the very latest in innovative hip joint technology to minimise the risk of dislocation and maximise your chances of returning to normal activities without complications.
Fracture:
Fractures can occur during or after the surgery, especially if you have weak or brittle bones.
Implant loosening:
The new implant may become loose over time, which can cause pain, instability, and the need for additional surgery.
Allergic reaction:
Some people may have an allergic reaction to the implant materials, other medical components (such as suture material), anaesthetic or medications.
Nerve or blood vessel damage:
In rare cases, the nerves or blood vessels near the hip joint may be damaged, which can cause pain, numbness, or other complications.
Don’t feel intimidated by this list. We will prescribe medications and exercises to reduce these risks. It is important to discuss risks and voice any concerns you may have with our team before having total hip replacement surgery.
What Will My Recovery Be Like?
Pre-surgery:
Preparation for your recovery begins before your surgery. We want you to be in the best physical condition to give you the most successful outcome so we will talk to you about reaching and maintaining a healthy body weight, keeping active and strengthening your hip muscles in the lead up to surgery. As a minimum, we ask that you attend a pre-operative assessment and education session with a physiotherapist. Ask our team for an appointment with our Physiotherapist Co-ordinator.
Day of surgery or the following day:
Post-operative physiotherapy begins.
1–3 days after surgery:
You will be discharged from hospital. To prepare you for going home, we aim to minimise pain and swelling, assist you to get in and out of bed, help you walk using crutches, and to manage stairs. You will also receive advice to minimise the risk of a fall or dislocation of your new hip.
3–4 weeks after surgery:
Your wound should be completely sealed. During this first month, you should avoid excessive bending, pivoting or twisting.
4–6 weeks after surgery:
You should be able to return to your normal activities.
12 months after surgery:
All being well, you should expect a total recovery by this stage.

